Gelrin is a patented hydrogel platform originally developed at the Technion – Israel Institute of Technology by Prof. Dror Seliktar. Itis a family of hydrogels that derive their unique physical and chemical properties from polymer chains crosslinked with trace quantities of denatured protein. In the body, Gelrin is eroded and resorbed over time through a pre-programmed and controlled gradual surface degradation process, meaning that the GelrinC implant covers the entire wound, so the cells that naturally want to migrate to the damaged tissue in situations where there is nothing holding them back or preventing them from migration, are unable to migrate due to the GelrinC implant and are controlled, which allows for the receding implant to allow the surrounding cells to regenerate the cartilage in a controlled and synchronous process.
The body of this receding mass acts to stimulate the body’s natural healing process, by guiding the migration and organization of cells involved in tissue repair doing so in a gradual process over time. Gelrin is applied in liquid form allowing it to completely fill the entire tissue defect and is then cured into a rubbery implant by the use of ultraviolet, or UV, light. It can be introduced into narrow bone crevices or large spaces, open or closed.
The Gelrin platform has several distinct features and benefits for tissue regeneration applications, including:
The development work is supported by the European Commission as part of the Seventh Framework Programme (FP7).
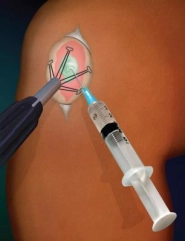 |
1. Stelar delivery device membrane covers cartilage lesion. Using a syringe GelrinC is introduced into the lesion. |
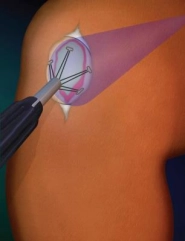 |
2. Upon filing of the lesion, UV beam cures GelrinC into a soft rubbery implant. |
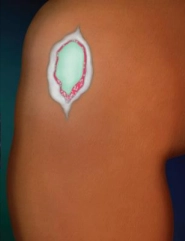 |
3. As GelrinC implant resorbs, the cartilage lesion rim creates aggregates and new cartilage tissue fills up the void created by the retreating |
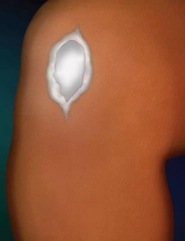 |
4. At the end of 6-9 months, GelrinC implant is resorbed, and new cartilage covers the treated lesion resulting in a functioning |
Regentis carried out a Pilot/Phase II study of 56 patients that were treated with GelrinC and followed up for up to four years in multiple sites in Northern Europe and Israel. The primary efficacy endpoints were superior changes from baseline for overall Knee injury and Osteoarthritis Outcome Score (KOOS) scores and KOOS pain subscale. The primary efficacy end points were met; the improvements observed in the (“KOOS”) and visual analog scale (“VAS”) pain measurement scores taken over two years were superior (100% greater improvement) to those seen with the traditional microfracture (the current “gold” standard) procedure. Additionally, patients continued to report further improvement and greater pain reduction of their knee and associated problems using GelrinC for four years. No serious adverse events were observed for the product in the completed Pilot study.
Based on these results, the FDA granted Regentis an investigational device exemption, or IDE, for our pivotal trial, permitting PMA submission with two-year follow-up data of 80 patients, with an additional 40 patients to be treated thereafter. The pivotal trial is currently being conducted in the United States and Europe, under the FDA’s sanctioned protocol, is an open label study, with one arm only (treatment), using our own historical control (microfracture). To-date, we have treated 47 patients out of the 80 initial patients.